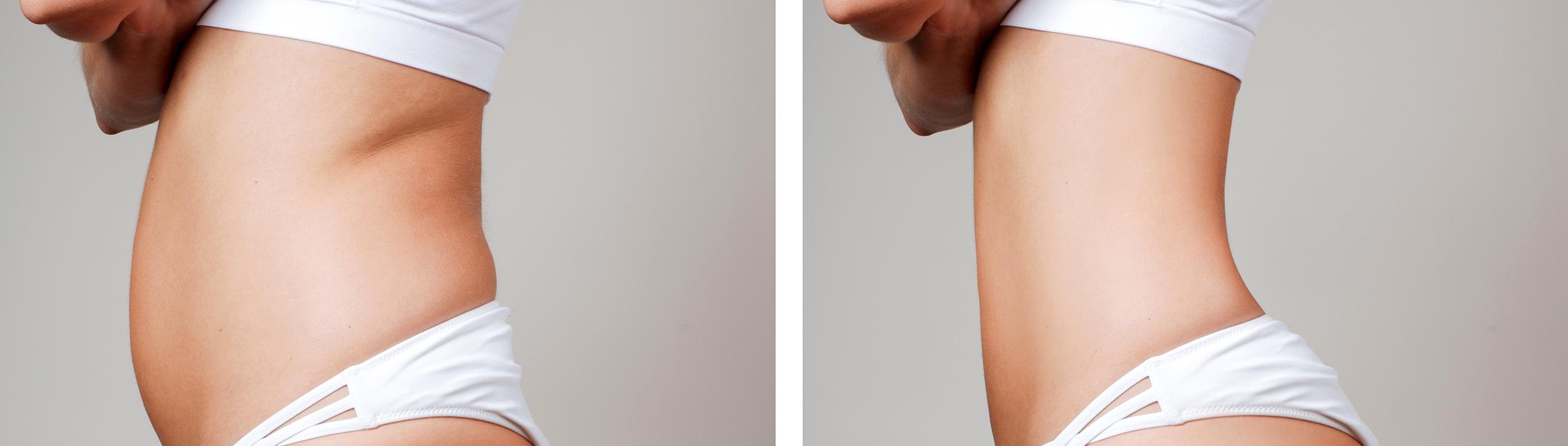
Gastric sleeve surgery, or sleeve gastrectomy, is surgery for weight loss that involves removal of a large part of the stomach. After the surgery, the person feels full after eating a small amount of food.
The surgery also makes people feel less hungry because a smaller stomach will produce lower levels of a hormone called ghrelin, which causes hunger.
Gastric sleeve surgery is a surgical treatment for obesity and medical conditions related to obesity. It’s only offered to qualified people who have serious medical conditions related to their obesity or are at high risk for developing them. Gastric sleeve surgery can improve and sometimes eliminate diseases, including:
• Insulin resistance and Type 2 diabetes.
• Hypertension and hypertensive heart disease.
• Hyperlipidemia (high cholesterol) and arterial disease.
• Nonalcoholic fatty liver disease and steatohepatitis.
• Obesity hypoventilation syndrome and obstructive sleep apnea.
• Joint pain and osteoarthritis.
What qualifies you for gastric sleeve surgery?
• That you have severe obesity (class III). This is determined by your BMI (body mass index), which is calculated by your weight and height, and your related health conditions. Class III obesity means a BMI of 40 or higher, or a BMI of at least 35 with at least one related disease.
• That you have tried to but not succeeded in losing weight prior to surgery. You may be required to spend three to six months on a medically supervised weight loss plan before your surgery.
• That you are physically and mentally prepared for the surgery and recovery process.
How do I get ready for gastric sleeve surgery?
Our surgeon will need to make sure that gastric sleeve surgery is a good option for you. Weight-loss surgery isn’t advised for people who abuse medicines or alcohol, or who are not able to commit to a lifelong change in diet and exercise habits. You’ll also need physical exams and tests. You will need blood tests. You may have imaging studies of your stomach or have an upper endoscopy. If you smoke, you will need to stop before surgery. Your surgeon may ask you to lose some weight before surgery. This will help make your liver smaller and make surgery safer. You’ll need to stop taking aspirin, ibuprofen, and other blood-thinning medicines in the days before your surgery. You shouldn’t eat or drink anything after midnight before surgery
Recovery after Surgery
• The surgery takes approximately 40-70 minutes
• Discharge from hospital typically occurs after 1-2 nights
• All patients are encouraged to walk as early as 3-4 hours after surgery
• In general, the pain is easily manageable after surgery. Most patients take less than the recommended pain medication
• Most patients go back to work and/or school after 2-4 weeks. Fatigue is common the first 2 weeks due to low calorie intake from liquid diet. However, the majority of patients do not feel hungry during this stage of the diet. The energy level improves quickly after the introduction of the soft diet, which is approximately 2 weeks after surgery. On occasion, we allow patients to work from home 2-3 days per week after surgery
• Patients can begin exercising 4 weeks after surgery
After the procedure
After sleeve gastrectomy, your diet begins with sugar-free, noncarbonated liquids for the first seven days, then progresses to pureed foods for three weeks, and finally to regular foods approximately four weeks after your surgery. You may need laboratory testing, bloodwork and various exams. You may experience changes as your body reacts to the rapid weight loss in the first three to six months after sleeve gastrectomy, including:
• Body aches
• Feeling tired, as if you have the flu
• Feeling cold
• Dry skin
• Hair thinning and hair loss
• Mood changes
Complications and Risks
Over the past decade, with the improvement of surgical techniques and surgeons’ experience, the gastric sleeve has become an overall safe bariatric surgical procedure. However, complications can still occur during and after surgery. Below are the main complications and risks of the gastric sleeve surgery:
• Leakage from the staple line – this is a rare complication of the gastric sleeve surgery. The stable line opens after surgery. Most leaks can be treated with endoscopic procedure.
• Stricture/stenosis – another rare complication with narrowing of the stomach after sleeve gastrectomy. Most stricture/stenosis can be treated with endoscopic dilation.
• Bleeding
• Blood Clot
• Heart Burn – This is a very controversial topic in bariatric surgery and the data from different centers is inconsistent. In our experience, most patients with heartburn before surgery see improvement of symptoms after surgery due to weight loss. Some patients may develop new heartburn, which is treatable with over-the-counter anti-acid medications, in most cases.
• Nutrient or vitamin deficiency
• Weight Regain – After 1-2 years, slight weight regain is common among all bariatric procedures and about 10-20% of patients can have significant weight regain after gastric sleeve surgery. After 5 years of follow up, many centers collected data to show that the majority of patients can maintain their weight loss after the Gastric Sleeve Surgery.
• Excess skin
What should I expect after the gastric sleeve as a result in long term?
Keep in mind the different variables that affect patients after gastric sleeve surgery. In the first year, patients usually lose weight no matter what. In year 2 thru 5 post-operation, adapting to a healthy lifestyle is critical because cravings slowly return and the body adjusts to the sleeve stomach. After year 5 and on, patients need to surround their environment with a healthy diet, positive nutrition, and physical activity. Every day needs to be a conscious decision to continue a healthy lifestyle. Patients must stay motivated and determined to stay healthy.
Weight gain after gastric sleeve surgery can happen at one time or another. These can start as stalls or plateaus, and grow into weight regaining if patients do nothing about it. After surgery, losing weight comes naturally and quickly. It feels like no matter how bad or good your eating habits are – patients still lose weight.
Causes of Weight Gain Include
• Overeating
• Bad nutrition habits
• Not taking vitamins
• Not eating proper amounts of fat or protein
• Side effects of medication If you are not losing weight after gastric sleeve, try to make adjustments based on things you can change. If a stall or plateau continues, you may consider looking into gastric sleeve revision surgery.
Stomach Stretching
One of the most common misconceptions after surgery is stretching the sleeve stomach from eating too much. Everyone asks, “Will my stomach stretch after surgery?” Most patients think if they eat too much, the stomach will stretch back to its original size.
Fortunately, that is not true. Yes, the stomach is an elastic organ meaning it can vary in size and stretch slightly. The amount it can stretch is very insignificant.
To Prevent Stomach Stretching After Gastric Sleeve
• Do not continuously snack throughout the day
• Keep track of portion size
• Do not eat impulsively
• Control stress, depression, and lack of sleep to the best of your ability
• Do not use eating as an outlet for negative emotions
• Do not overuse sugar-filled or artificially sweetened drinks
• Ask your doctor or primary physician about changes in medications if they increase hunger
© COPYRIGHT 2022 ALL RIGHTS RESERVED | BELLADONNA.

